Guide
How Long Does Sciatica Last? (Recovery Timeline)
How long does sciatica last? Most acute cases resolve in 4-6 weeks. Chronic sciatica lasts 3+ months. Full recovery timelines, stages, and when to see a doctor. 2026.
By Dr. Michael Torres, Physiotherapist | Last updated: March 21, 2026
This article is for informational purposes only. Consult a healthcare provider for diagnosis and treatment.
Most acute sciatica cases resolve within 4–6 weeks with appropriate conservative treatment. Approximately 90% of patients recover significantly within 12 weeks without surgery. Chronic sciatica — defined as symptoms persisting beyond 12 weeks — affects 20–30% of cases and requires more targeted intervention. Understanding which stage you are in is the key to managing expectations and choosing the right treatment approach.
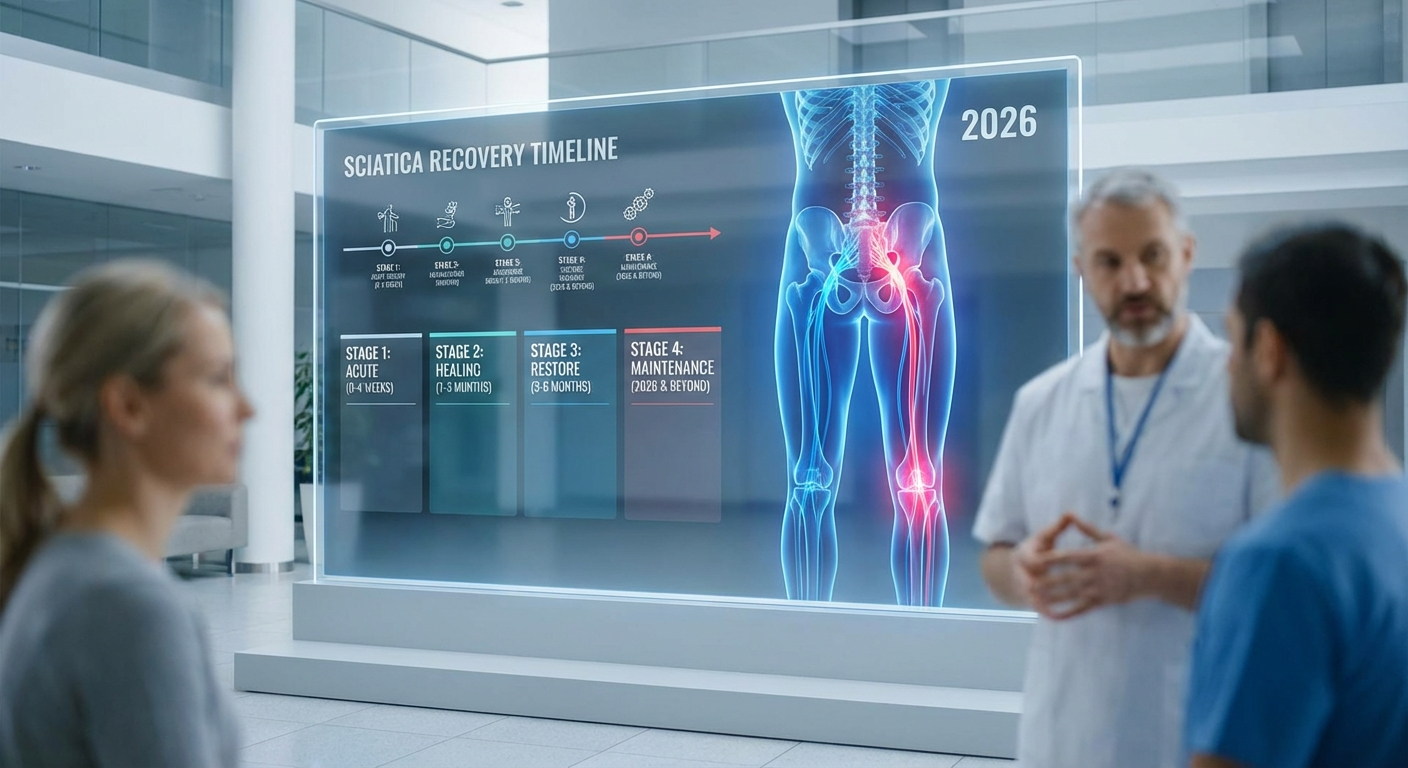
Table of Contents
- Sciatica Recovery Timeline: What to Expect Week by Week
- Acute vs Chronic Sciatica: Key Differences
- Signs Your Sciatica is Healing
- What Makes Sciatica Last Longer
- Treatment Approaches by Duration Stage
- When to See a Doctor
- Sciatica Recovery by Cause
- Frequently Asked Questions
- Sources & Methodology
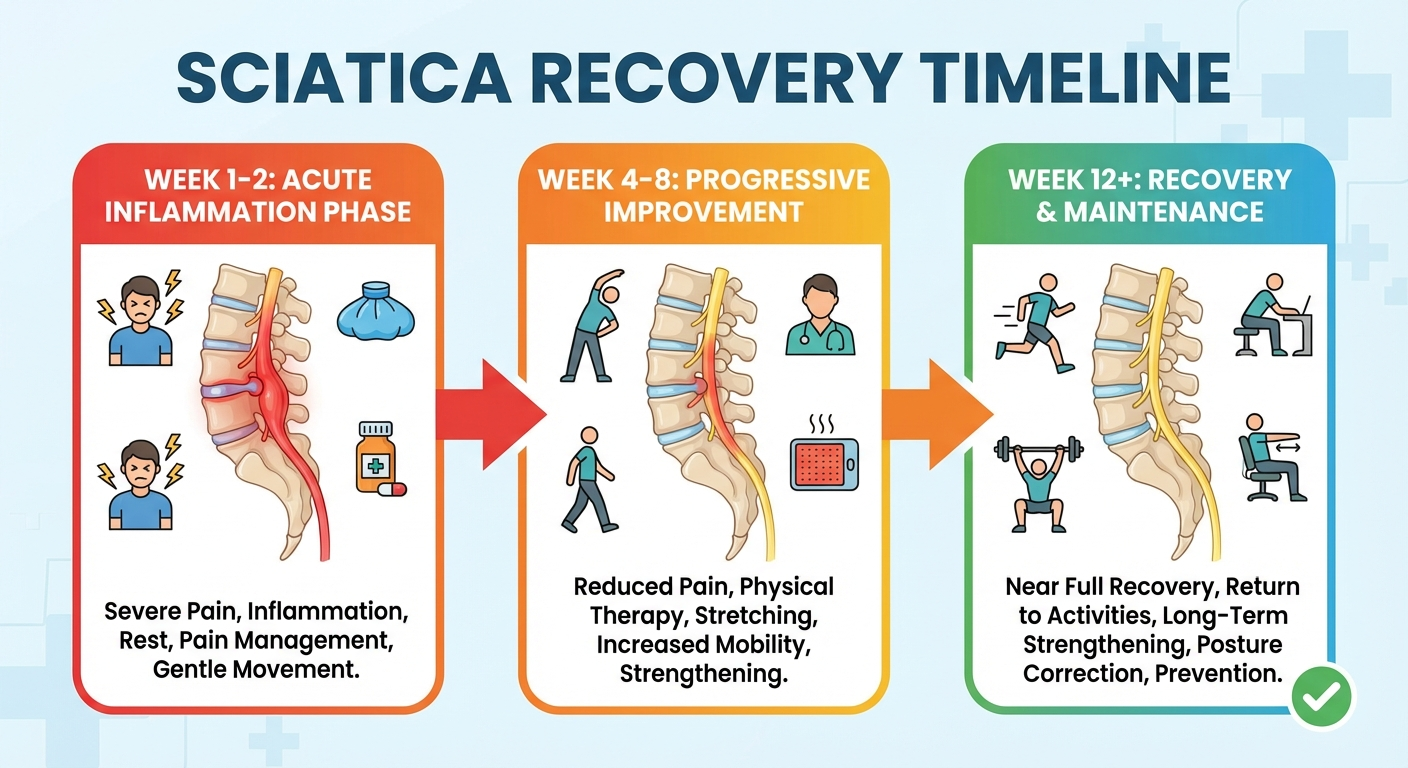
Sciatica Recovery Timeline: What to Expect Week by Week
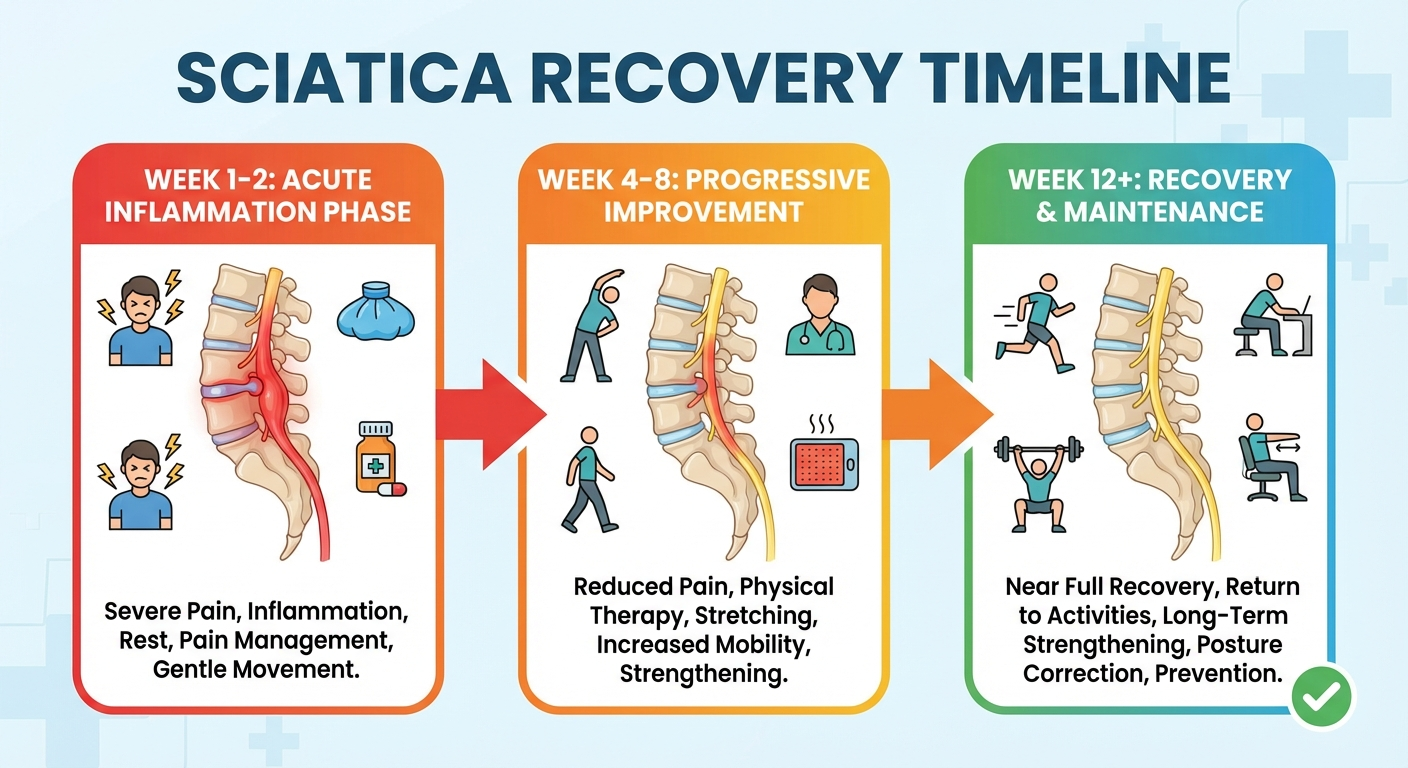
Week 1-2: Acute Phase (Inflammation Peak)
The first two weeks are typically the most painful. Inflammation around the compressed sciatic nerve root is at its highest. You may experience:
- Severe pain radiating from the lower back through the buttock and down the leg
- Pain worsened by sitting, coughing, or sneezing
- Numbness or tingling in the thigh, calf, or foot
- Reduced ability to perform daily activities
What to do: Alternate rest with gentle movement. Bed rest beyond 48 hours delays recovery — short walks (10-15 minutes) maintain circulation without aggravating the nerve. Ice for the first 48-72 hours to reduce inflammation, then transition to heat.
What not to do: Do not attempt forceful stretching or exercise during this phase. Do not remain seated for extended periods — standing or gentle walking is better than prolonged sitting.
Week 2-4: Early Recovery Phase
For most patients, pain intensity begins decreasing around week 2-3. Key positive signs:
- Centralization: Pain begins shifting from the foot/calf upward toward the lower back. This is the most reliable predictor of continued recovery.
- Leg pain becoming intermittent rather than constant
- Ability to walk longer distances
- Improved sleep duration
Approximately 50-60% of acute sciatica patients reach this positive trajectory by week 3. The remaining 40-50% show slower progress but still recover with conservative management.
Week 4-8: Progressive Improvement Phase
By week 4-8, most patients with acute sciatica can:
- Return to light work activities
- Walk 30-60 minutes without significant exacerbation
- Tolerate gentle physical therapy exercises
- Reduce dependence on pain medication
Research published in the New England Journal of Medicine (2007) found that at 4 weeks, patients receiving conservative treatment showed improvements in pain and function equivalent to those receiving early surgery.
Week 8-12: Return to Function
For patients recovering on schedule (the majority), weeks 8-12 typically bring:
- Return to most normal activities
- Residual ache rather than sharp radiating pain
- 70-80% function restored
- Ability to return to most work activities
By 12 weeks, approximately 90% of patients have made sufficient recovery to avoid surgical intervention. The small percentage remaining in significant pain at 12 weeks represents the chronic group requiring specialist evaluation.
Acute vs Chronic Sciatica: Key Differences
| Feature | Acute Sciatica | Chronic Sciatica |
|---|---|---|
| Duration | Under 12 weeks | 12+ weeks |
| Prevalence | 70-80% of cases | 20-30% of cases |
| Primary cause | Disc herniation, inflammation | Ongoing compression, stenosis |
| Natural recovery rate | 90% without surgery | 50-70% with active treatment |
| Treatment approach | Conservative (rest, ice/heat, gentle movement) | Physical therapy, injections, possible surgery |
| Work impact | Often 2-6 weeks off work | May require work modification |
Chronic Sciatica Defined
Sciatica is classified as chronic when significant symptoms persist beyond 12 weeks. Chronic sciatica does not mean permanent — many patients with chronic sciatica eventually recover fully with appropriate treatment. However, chronic cases typically require:
- Structured physical therapy programs (not just home exercises)
- Medical evaluation for underlying causes (MRI to identify herniation, stenosis, or other structural issues)
- Consideration of epidural steroid injections for pain control during rehabilitation
- Assessment for surgical candidacy if conservative treatment has failed at 6+ months
Signs Your Sciatica is Healing
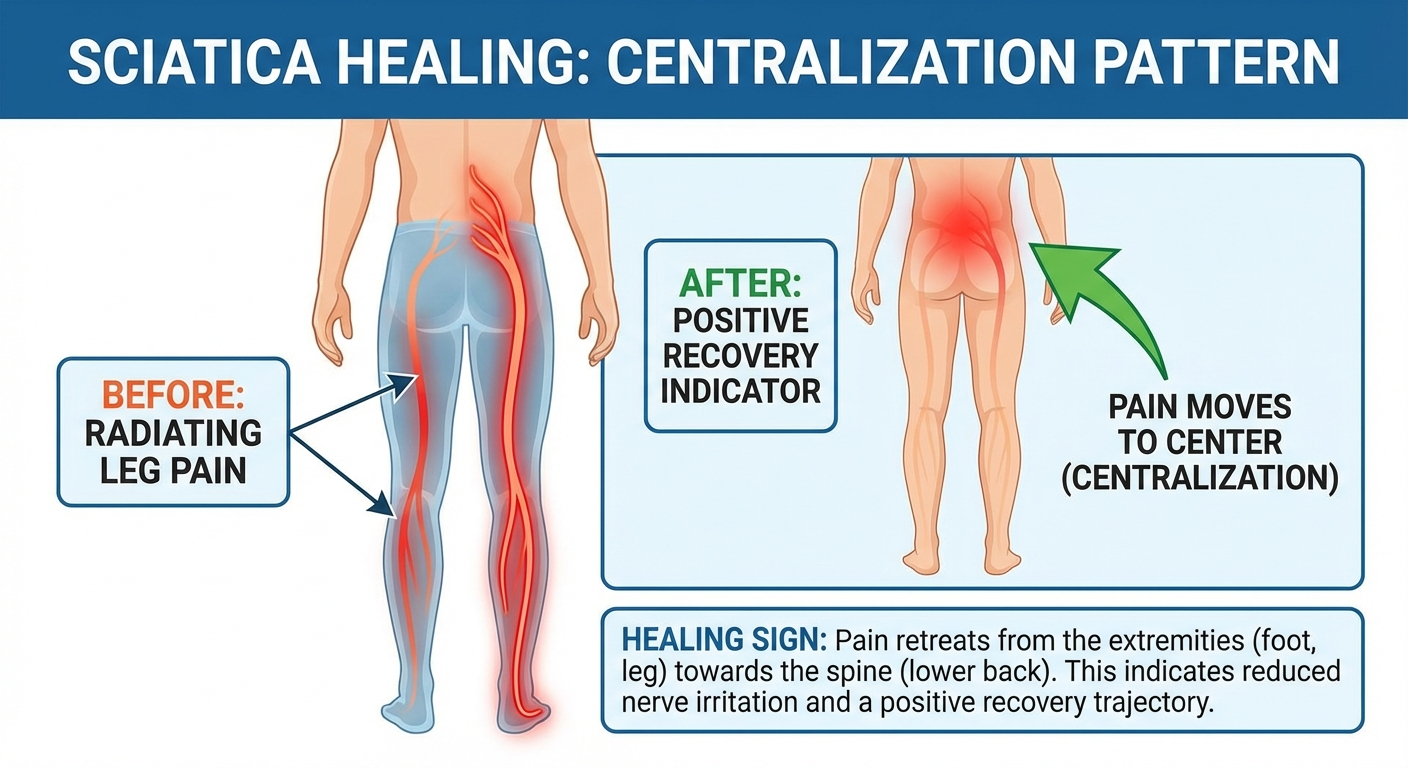
The Most Reliable Sign: Centralization
The single most predictive sign of sciatica recovery is pain centralization — the phenomenon where pain that was radiating into the foot or lower calf begins moving upward toward the buttock and lower back. This may initially feel like your back is getting worse, but centralization almost always means the nerve is decompressing.
Research published in the Journal of Manipulative and Physiological Therapeutics found that centralization predicted full recovery with 91% accuracy in patients who experienced it.
Other Positive Recovery Indicators
- Leg pain resolving faster than back pain — The radiating component typically clears before the central lumbar pain
- Pain becoming time-limited — Was constant, now only 2-4 hours per day
- Increased tolerance for walking — Can walk 20+ minutes without worsening
- Improved morning function — Morning stiffness resolving within 30 minutes
- Better sleep position tolerance — Can sleep through the night without waking from pain
- Reduced pins and needles — Tingling and numbness decreasing in the foot
Warning Signs (Not Healing)
Conversely, see your doctor if you notice:
- Pain spreading further down the leg (peripheralization — the opposite of centralization)
- Increasing weakness in the leg or foot
- New numbness in the groin or inner thighs (saddle anesthesia)
- Loss of bladder or bowel control (seek immediate emergency care)
- Both legs becoming symptomatic
What Makes Sciatica Last Longer
Certain factors significantly extend sciatica recovery time. Understanding these helps you avoid recovery-delaying behaviors:
Physical Factors
Prolonged sitting — The seated position increases intradiscal pressure by 40% compared to standing, compressing the herniated disc further against the nerve. Office workers who cannot modify their work posture frequently see delayed recovery.
Bed rest beyond 48 hours — Counterintuitively, complete bed rest beyond 2 days slows recovery. A 1986 New England Journal of Medicine study found that patients returning to activity within 48 hours recovered faster than those who maintained strict bed rest.
Weight and BMI — Higher BMI is associated with prolonged sciatica recovery. Excess weight increases lumbar disc loading and reduces the body's natural ability to reabsorb disc herniation material.
Behavioral Factors
Avoiding movement due to fear — Fear-avoidance behavior (avoiding all activity to protect against pain) leads to deconditioning that extends recovery. Graded exposure to activity — starting with gentle walking and progressively increasing — consistently outperforms strict rest.
Inconsistent treatment — Irregular physical therapy, sporadic exercise compliance, or stopping treatment prematurely at first sign of improvement leads to relapse.
Structural Factors
Spinal stenosis — Unlike disc herniation, which often resolves as disc material is reabsorbed, stenosis (narrowing of the spinal canal) is structural and typically does not improve spontaneously. Sciatica from stenosis tends to follow a more chronic course.
Multiple level involvement — Sciatica from a single disc level typically recovers faster than multi-level compression. MRI findings of L4-L5 and L5-S1 involvement simultaneously indicate a more complex presentation.
Treatment Approaches by Duration Stage

Everlasting Comfort Seat Cushion
Best for: Reducing sitting pressure during acute recovery
Stage: Weeks 1-8, office/car use
Check on Amazon →
Sunbeam King-Size Heating Pad
Best for: Heat therapy during weeks 2-12
Stage: After first 48-72 hours of ice
Check on Amazon →
Mueller Lumbar Support Back Brace
Best for: Work support during recovery weeks 3-8
Stage: Return to work activities
Check on Amazon →Weeks 1-4: Conservative Management
- Rest + gentle movement: Short walks (10-15 min, 3-4x/day) better than bed rest
- Ice then heat: Ice for first 48-72 hours, heat thereafter
- NSAIDs: Ibuprofen or naproxen if appropriate for pain and inflammation
- Positioning: Side-lying with knees bent and pillow between knees reduces nerve tension
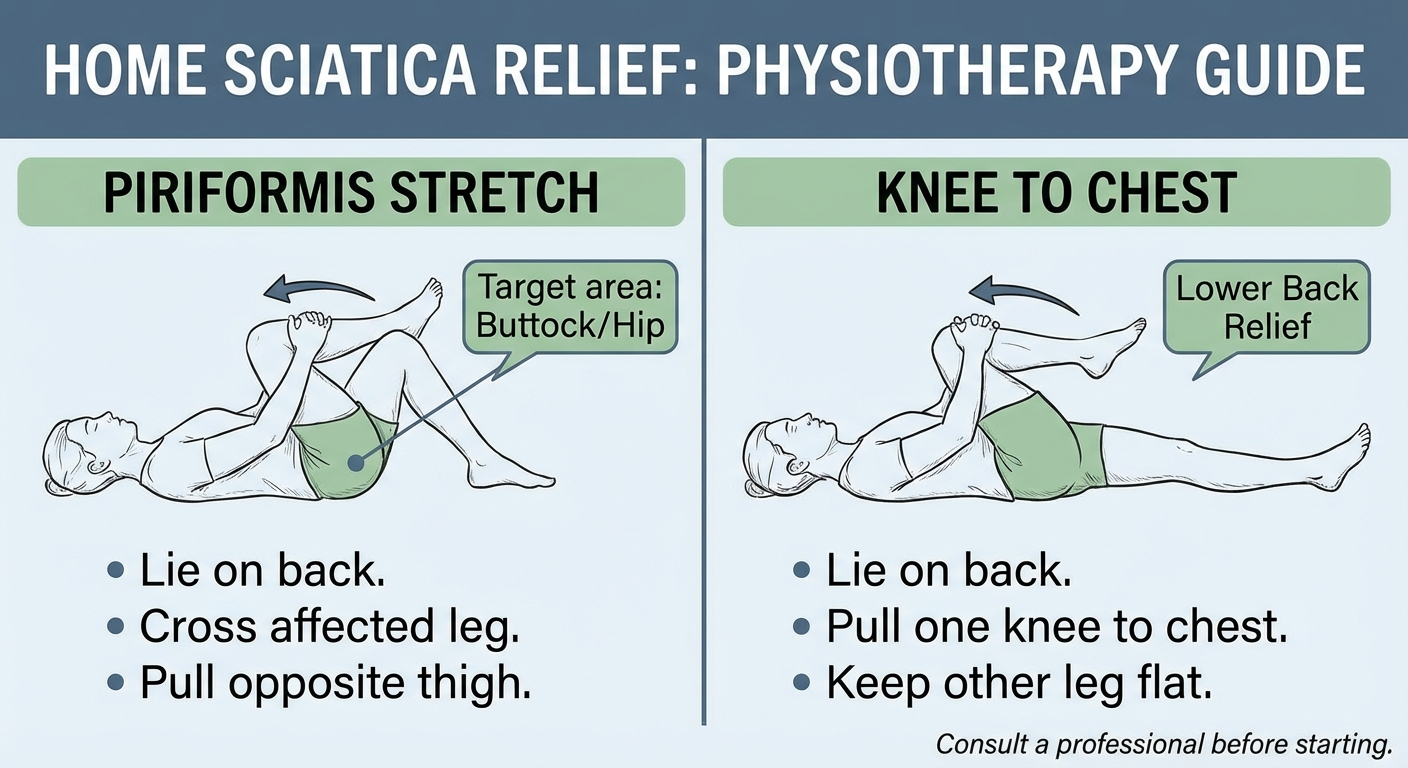
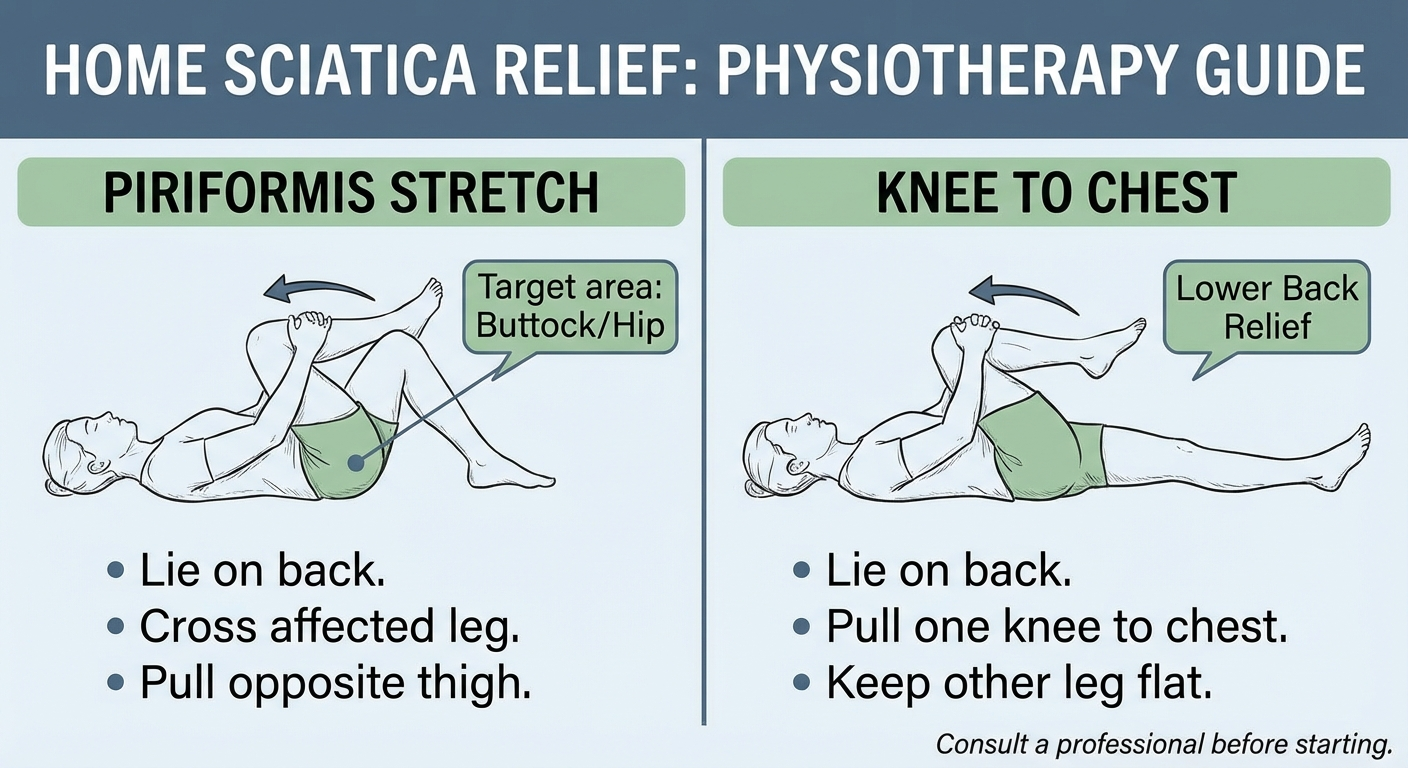
- Gentle stretches: Piriformis stretch, knee-to-chest (see our sciatica exercises guide)
Weeks 4-12: Active Rehabilitation
- Physical therapy: McKenzie Method has strongest evidence for disc-related sciatica
- Core strengthening: Gradual introduction of stabilization exercises
- Return to activity: Progressive increases in walking distance and daily activities
- Sleep positioning: Best sleeping positions for sciatica can significantly reduce nighttime pain
12+ Weeks: Chronic Management
- Epidural steroid injections: Provide short-term pain relief during intensive rehabilitation
- Continued physical therapy: Structured 12-week program with reassessment
- Surgical evaluation: Discectomy has strong evidence for disc-related sciatica persisting beyond 6 months
- Pain management team: For complex cases, multi-disciplinary approach
Also note: tailbone pain often accompanies sciatica recovery — coccyx support and positioning adjustments can address both symptoms simultaneously during rehabilitation.
When to See a Doctor
Seek Immediate Emergency Care (Same Day)
- Loss of bladder or bowel control
- Numbness in the groin, inner thighs, or genital area (cauda equina syndrome)
- Progressive foot drop (inability to lift the front of the foot)
- Sciatica following direct trauma or injury to the spine
See Your Doctor This Week
- Sciatica showing no improvement after 4 weeks of conservative treatment
- Severe pain preventing any normal activity
- Both legs affected
- Consistent worsening (not just fluctuating) over 2+ weeks
- Age over 70 with new-onset sciatica
- History of cancer, osteoporosis, or steroid use
Standard Timeline Check-In
If you've had sciatica symptoms for 6-8 weeks with gradual but incomplete improvement, schedule a routine medical appointment to:
- Confirm the diagnosis (rule out other causes of leg pain)
- Discuss imaging if indicated
- Review treatment plan and consider physiotherapy referral
Sciatica Recovery by Cause
Not all sciatica is equal. Recovery timelines vary significantly based on the underlying cause:
| Cause | Typical Recovery Time | Surgery Rate | Notes |
|---|---|---|---|
| Disc herniation (L4-L5 or L5-S1) | 6-12 weeks | 5-10% | Disc reabsorption supports natural recovery |
| Piriformis syndrome | 4-8 weeks | Rare | Responds well to physical therapy |
| Lumbar spinal stenosis | Variable (months-years) | 20-30% | Structural; less natural resolution |
| Degenerative disc disease | Variable | 10-20% | Age-related; management focus |
| Spondylolisthesis | 8-16 weeks | 15-25% | Vertebral slip; stability focus |
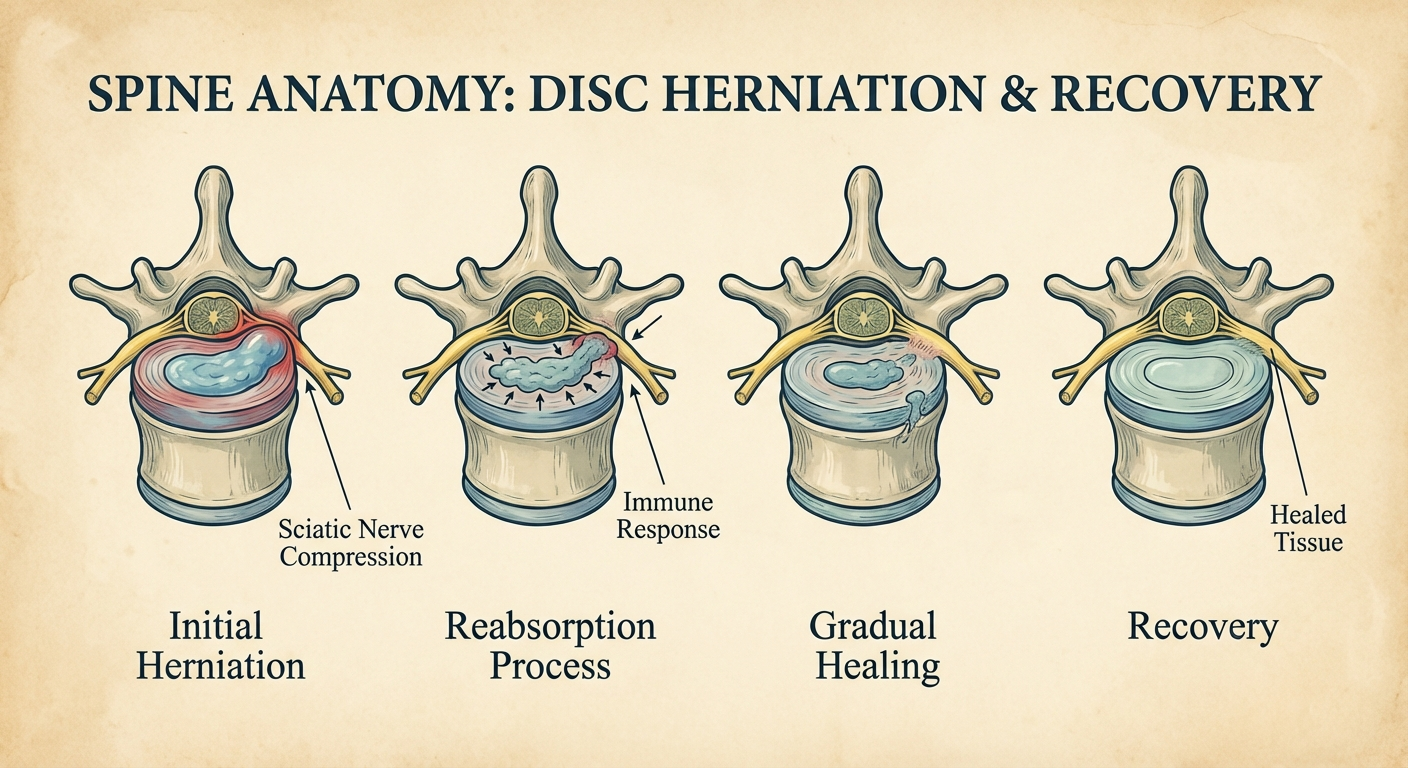
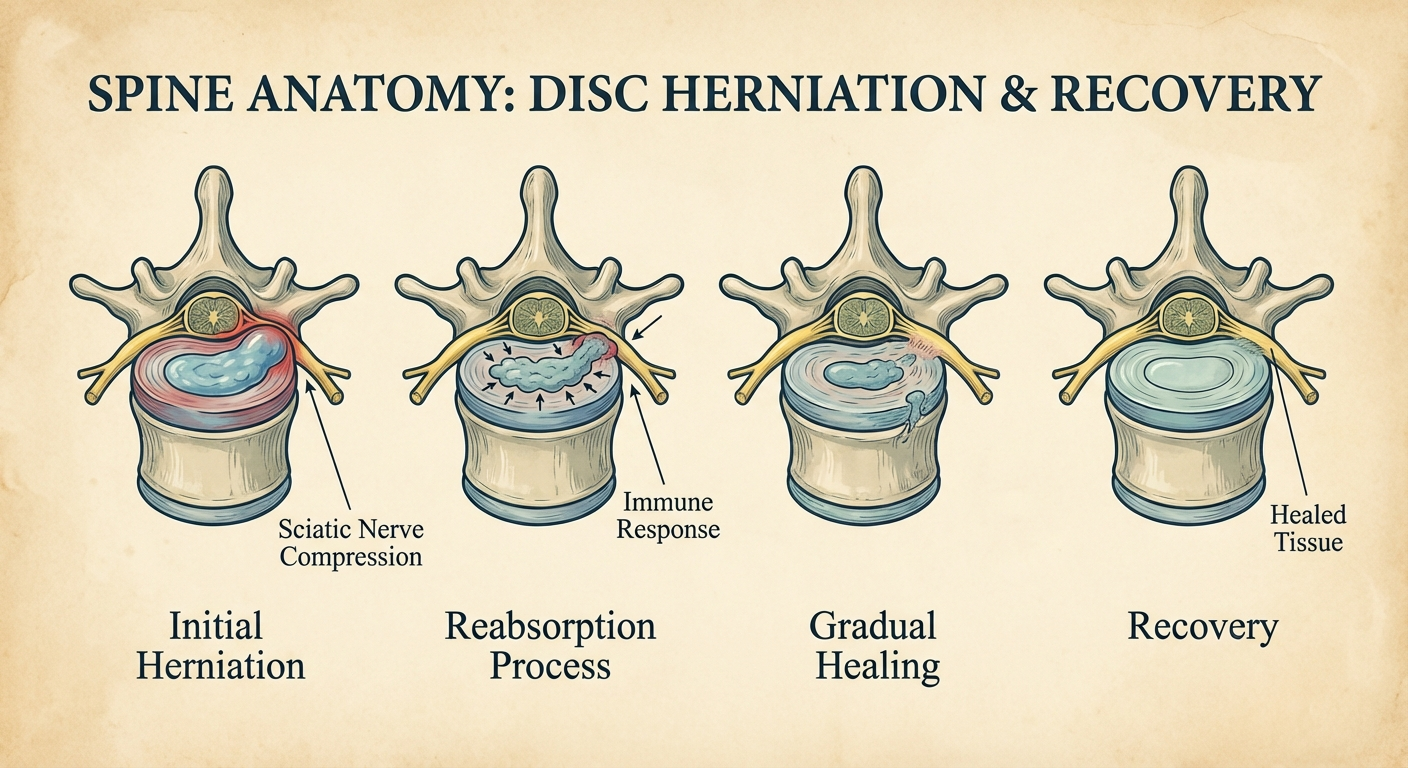
For disc herniation (the most common cause), imaging studies consistently show that herniations decrease in size over time in 90%+ of cases, even without surgery. The body's reabsorption mechanism is the primary driver of natural recovery.
Frequently Asked Questions
How long does sciatica last on average?
Most acute sciatica resolves within 4-6 weeks. 90% of cases recover significantly within 12 weeks without surgery. Chronic sciatica (12+ weeks) affects 20-30% of patients.
Can sciatica go away on its own?
Yes — research shows 90% of disc-related sciatica resolves spontaneously within 12 weeks. Conservative management (gentle movement, heat/ice, anti-inflammatories) supports natural recovery.
How do I know if my sciatica is healing?
The most reliable sign is centralization — pain shifting from the foot/calf upward toward the lower back. Other positive signs include reduced intensity, intermittent rather than constant pain, and improved walking tolerance.
What is the fastest way to recover from sciatica?
Stay active with gentle movement (avoid prolonged bed rest), use heat after the first 48 hours, do targeted stretches like the piriformis stretch, and consider physical therapy using the McKenzie Method for disc-related sciatica.
When should I worry about sciatica?
Seek immediate care for bladder/bowel changes, progressive leg weakness, or bilateral symptoms. See your doctor within a week if symptoms don't improve after 4 weeks, worsen consistently, or are severe.
Does sciatica get worse before it gets better?
Mild initial worsening in the first 1-2 weeks is common as inflammation peaks. However, consistent worsening over more than 2 weeks warrants medical evaluation.
Sources and Methodology
Medical References:
- Koes BW et al: "Diagnosis and treatment of sciatica." BMJ 2007 — foundational systematic review on conservative vs surgical outcomes
- Van Tulder MW et al: European Spine Journal systematic review on disc herniation natural history 2012
- Waddell G et al: "A Fear-Avoidance Beliefs Questionnaire" — spine research on activity avoidance and recovery delays
- Deyo RA et al: NEJM 1986 — bed rest versus early activity in low back pain
- Jensen MC et al: NEJM 1994 — MRI findings of disc abnormalities in asymptomatic subjects
Terminology:
- "Sciatica" as used here refers to radiculopathy from L4-S1 nerve root compression
- Recovery percentages based on systematic review data; individual outcomes vary
- This article is informational only; consult a healthcare provider for personal medical advice
Internal links referenced:
For additional pain relief during recovery, consider a memory foam seat cushion for sciatica for long sitting sessions and a TENS unit for nerve pain for at-home pain management between physical therapy sessions.